Lyme Disease
Lyme disease
What Is Lyme Disease?
Lyme disease is a bacterial infection transmitted by ticks. and was first recognized in 1975, after researchers investigated why unusually large numbers of children were being diagnosed with juvenile rheumatoid arthritis in Lyme, Connecticut (and two neighboring towns).
Investigators discovered that most of the affected children lived near wooded areas likely to harbor ticks and that the children’s first symptoms typically started in the summer months coinciding with the height of the tick season.
Several patients reported having a peculiar skin rash just before developing arthritis symptoms, and many also recalled being bitten by a tick at the rash site.
Further investigations resulted in the discovery that tiny deer ticks infected with a spiral-shaped bacterium or spirochete (which was later named Borrelia burgdorferi) were responsible for the outbreak of arthritis in Lyme. Ordinary “wood ticks” and “dog ticks” do not carry the infection.
The ticks most commonly infected with B. burgdorferi usually feed and mate on deer during part of their life cycle. The recent growth of the deer population in the northeast and the building of suburban developments in rural areas where deer ticks are commonly found have probably contributed to the increasing number of people with the disease.
The number of reported cases of Lyme disease, as well as the number of geographic areas in which it is found, has been increasing. Lyme disease has been reported in nearly all states in this country, although most cases are concentrated in the coastal northeast, Mid-Atlantic States, Wisconsin, and Minnesota, and northern California. Lyme disease is also found in large areas of Asia and Europe. Recent reports suggest that it is present in South America, too.
In addition to causing arthritis, Lyme disease can also cause heart, brain, and nerve problems.
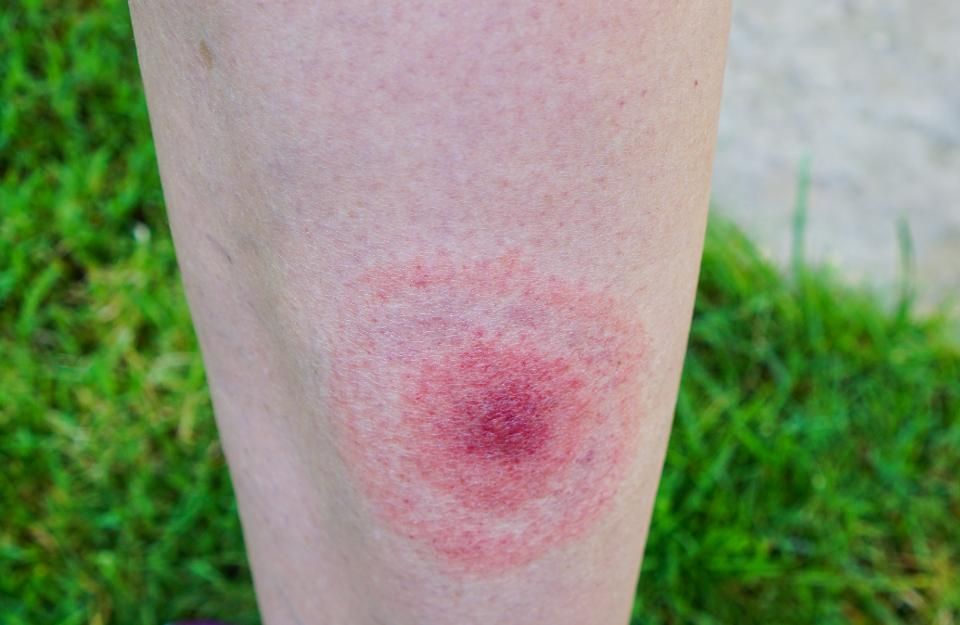
Ring Rash?
If you or your child has a rash that looks like this, please contact us immediately! This is one of the primary indicators of Lyme Disease.
SYMPTOMS
In the early stages of Lyme disease, you may experience flu-like symptoms that can include a stiff neck, chills, fever, swollen lymph nodes, headaches, fatigue, muscle aches, and joint pain. You also may experience a large, expanding skin rash around the area of the tick bite. In more advanced disease, nerve problems and arthritis, especially in the knees, may occur.
Here are some more details:
-
Erythma migrans. Erythema migrans is the telltale rash which occurs in about 70% to 80% of cases and starts as a small red spot that expands over a period of days or weeks, forming a circular, triangular, or oval-shaped rash. Sometimes the rash resembles a bull’s-eye because it appears as a red ring surrounding a central clear area. The rash, which can range in size from that of a dime to the entire width of a person’s back, appears between three days and a few weeks of a tick bite, usually occurring at the site of a bite. As infection spreads, several rashes can appear at different sites on the body.
Erythema migrans is often accompanied by symptoms such as fever, headache, stiff neck, body aches, and fatigue. These flu-like symptoms may resemble those of common viral infections and usually resolve within days or a few weeks.
-
Arthritis. After several weeks of being infected with Lyme disease, approximately 60% of those people not treated with antibiotics develop recurrent attacks of painful and swollen joints that last a few days to a few months. The arthritis can shift from one joint to another; the knee is most commonly affected and usually one or a few joints are affected at any given time. About 10% to 20% of untreated patients will go on to develop lasting arthritis. The knuckle joints of the hands are only very rarely affected.
-
Neurological symptoms. Lyme disease can also affect the nervous system, causing symptoms such as stiff neck and severe headache (meningitis), temporary paralysis of facial muscles (Bell’s palsy), numbness, pain or weakness in the limbs, or poor coordination. More subtle changes such as memory loss, difficulty with concentration, and a change in mood or sleeping habits have also been associated with Lyme disease. People with these latter symptoms alone usually don’t have Lyme disease as their cause.
Nervous system abnormalities usually develop several weeks, months, or even years following an untreated infection. These symptoms often last for weeks or months and may recur. These features of Lyme disease usually start to resolve even before antibiotics are started. Patients with neurologic disease usually have a total return to normal function.
-
Heart problems. Fewer than one out of 10 Lyme disease patients develops heart problems, such as an irregular, slow heartbeat, which can be signaled by dizziness or shortness of breath. These symptoms rarely last more than a few days or weeks. Such heart abnormalities generally appear several weeks after infection, and usually begin to resolve even before treatment.
-
Other symptoms. Less commonly, Lyme disease can result in eye inflammation and severe fatigue, although none of these problems is likely to appear without other Lyme disease symptoms being present.
Lyme disease imitates a variety of illnesses and its severity can vary from person to person. If you have been bitten by a tick and live in an area known to have Lyme disease, see your doctor right away so that a proper diagnose can be made and treatment started
HOW IS LYME DISEASE DIAGNOSED?
Lyme disease may be difficult to diagnose because many of its symptoms mimic those of other disorders. Although a tick bite is an important clue for diagnosis, many patients cannot recall having been bitten by a tick. This is not surprising because the tick is tiny, and a tick bite is usually painless.
The easiest way for a doctor to diagnose Lyme disease is to see the unique bull’s-eye rash. If there is no visible rash (as is the case in about one-fourth of those infected), the doctor might order a blood test three to four weeks after the onset of the suspected infection to look for antibodies against the bacteria. Unfortunately, the Lyme disease bacterium itself is difficult to isolate or culture from body tissues or fluids. These blood tests are:
-
ELISA. This blood test measures the levels of antibodies against the Lyme disease bacteria that are present in the body. Antibodies are molecules or small substances tailor-made by the immune system to lock onto and destroy specific microbial invaders.
-
Western blot. This blood test identifies antibodies directed against a panel of proteins found on the Lyme bacteria. The test is ordered when the ELISA result is either positive or uncertain.
The presence of antibodies, however, does not prove that the bacterium is the cause of a patient’s symptoms. The presence of specific antibodies suggests a prior infection, which may or may not still be active.
Note: In the first few weeks following infection (when the rash first appears), antibody tests are not reliable because a patient’s immune system has not produced enough antibodies to be detected. Antibiotics given to a patient early during infection may also prevent antibodies from reaching detectable levels, even though the Lyme disease bacterium is the cause of the patient’s symptoms.
Other Testing. Some patients experiencing nervous system symptoms may also undergo a spinal tap. A spinal tap is a procedure in which spinal fluid is removed from the spinal canal for the purpose of diagnosis in a laboratory. Through this procedure, doctors can detect brain and spinal cord inflammation and can look for antibodies against the Lyme disease bacterium in the spinal fluid.
LYME DISEASE TREATMENT OPTIONS?
In its early stages, Lyme disease can be effectively treated with antibiotics. In general, the sooner such therapy is begun following infection, the quicker and more complete the recovery. Antibiotics, such as doxycycline or amoxicillin taken orally for two to four weeks, can speed the healing of the rash and can usually prevent subsequent symptoms such as arthritis or neurological problems. There is no compelling evidence that prolonged antibiotic therapy is more effective than two weeks of therapy. Prolonged antibiotic use may have serious side effects.
Intravenous (IV) antibiotics may be used for more serious cases and for someone whose nervous system has been affected. Lyme disease with arthritis also can be treated with antibiotics. Most patients experience full recovery.
Patients younger than 9 years or pregnant or lactating women with Lyme disease are treated with amoxicillin or penicillin because doxycycline can stain the permanent teeth developing in young children or unborn babies. Patients allergic to penicillin are given erythromycin or related antibiotics.
Doctors prefer to treat Lyme disease patients experiencing heart symptoms with antibiotics such as Rocephin, Claforan, or penicillin given intravenously for about two weeks. If these symptoms persist or are severe enough, patients may also be treated with corticosteroids or given a temporary internal cardiac pacemaker. People with Lyme disease rarely experience long-term heart damage.
Following treatment for Lyme disease, some people still have persistent fatigue and achiness. This general malaise can take months to slowly disappear, although it generally does so spontaneously without the use of additional antibiotic therapy. There is no evidence that the Borrelia infection causes systemic exertion intolerance disease (formerly called chronic fatigue syndrome) or fibromyalgia. Although some patients with Lyme disease may develop these problems, as with other patients who get SEID or fibromyalgia, long-term antibiotics will not hasten recovery.
A new, innovative treatment for pain associated with Chronic Lyme Disease is IV Ketamine Infusions. At Pain MD Houston, Dr. Mukalel’s treatment protocols are individually planned depending on the nature of the patient’s pain and responsiveness to initial sessions. Infusion cocktails are prepared in-house so that they can be tailored to each patient’s therapeutic needs.
